The cumbersome and inefficient format of clinical trials leads to billions lost in dead-end product research every year: the price paid for safe and effective drugs.
However, new technologies and advancements in the understanding of what makes people tick both mentally and physically show some promise in the effort to streamline, improve and advance this process.
The future of clinical trials looks to be one driven by powerful, predictive AI, facilitated by wireless implants and smart technologies, and focusing on patient experience as part of the process. Every industry involved in these three disciplines is on a rapidly advancing trajectory, and this suggests good things for future clinical research as a whole.
However, it will take some shifts in attitudes, and a significant investment to make the change in the near future. Let’s take a look at why.
The Current State Clinical Trials
To set a baseline for comparison, it’s useful to pull out the figures. While you’ll be familiar with the way trials are run, it might be less obvious just how much they cost or how long they take. So, starting from the very beginning, let’s do a brief overview of the process.
Clinical trials obviously aren’t the start of the clinical research process. From the discovery of potentially useful compounds, preclinical trials are conducted on animals. This process can take up to six years, and for every 10,000 compounds discovered, perhaps only 250 will make it to animal testing.
Once these animal tests are complete, successful drugs will be deemed fit for future clinical trials on humans.
The basic framework for testing drugs on human participants follows four phases.
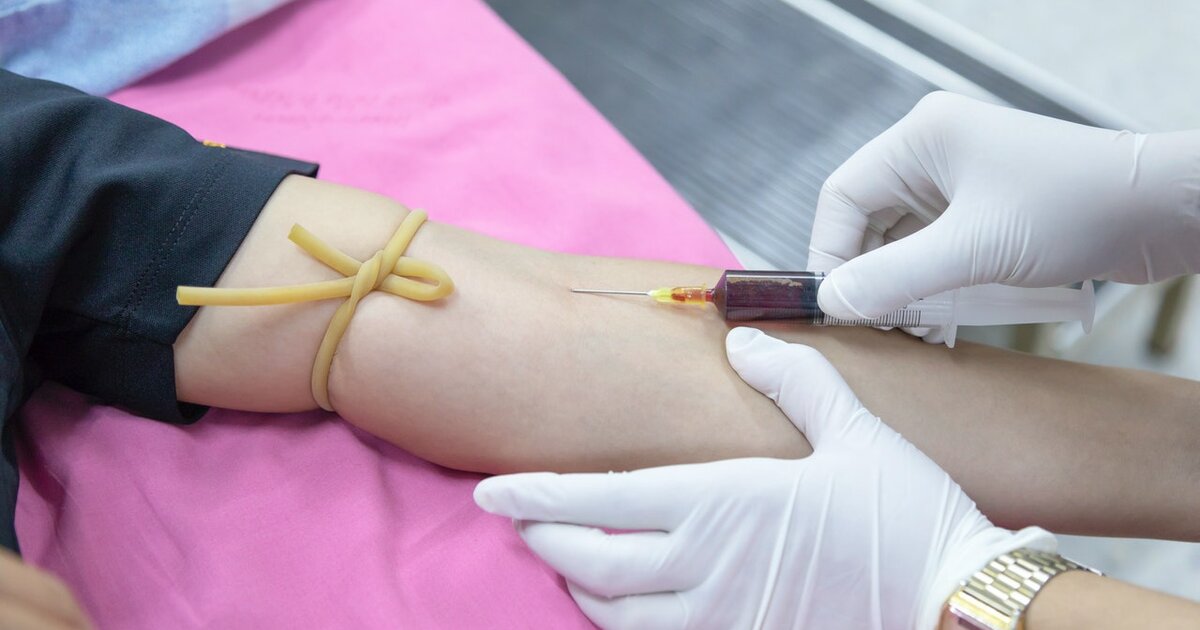
- Phase 1 – You can expect somewhere between 20 and 200 volunteers to enter phase 1 clinical trials. While this is the first level of testing on humans and involves the smallest sample sizes, phase 1 testing can cost up to and over $6 million.
- Phase 2 – between 100 and 500 participants might be involved in phase 2 trials, which revolve around checking the efficacy of the drug. Participants will usually receive payment for taking part in this stage and it will be more expensive than phase 1 to conduct, costing up to around $20 million.
- Phase 3 – is the reinforcement stage, and costs more again than phase 2. In this stage, samples need to be one hundred times greater, meaning 1000 to 5000 participants will be involved. Now we’re looking at costs of up to around $50 million, depending on the drug type.
- Phase 4 – involves continued surveillance for safety as the drug goes live, and follows prolonged usage among patients. This is where the FDA will review the long-term efficacy and safety of the drug, and their involvement isn’t cheap either. With all the follow-up and licensing, certain drugs can cost $73 million to push through phase 4 testing.
In general, you’re looking at somewhere between $40 million and $120 million, depending on the drug type. So, these studies are expensive, require huge amounts of human and professional resources, and take a long time to complete.
On top of all this, most end in failure. The FDA states that only around 7% of drugs move through all four of these phases to FDA approval, and this can be after a lengthy process of drug discovery, through pre-clinical before even reaching Phase 1 of clinical trials; something which can take up to six years. Then, clinical trials themselves can take a further six to seven years to complete.
One other significant challenge is participant retention. The longevity, discomfort, and unstimulating experiences that participants face lead to high levels of drop-out, and can often destroy a trial simply through the unviable sample size.
Management is also an issue, as it relates to follow-up, subjective reporting, and tracking of all the participants in the trial. Location is a big one, too. Accessing candidates, and then treating and following up are all hindered by the costs and encumberments of reaching affected populations effectively.
For any number of these reasons, a trial may fail. In the worst-case scenario, this means you’re looking at the possibility of up to fifteen years of research to find out that a drug isn’t viable.
So, there’s significant motivation from numerous sectors to improve the process and lessen the financial and human burden on the process, as well as improve the time it takes to get life-saving drugs to market, and the overall quality of the products of these trials.
In order to make improvements in this regard, industries are looking to psychology, tech, and AI.
The Role of Psychology in the Future of Clinical Trials
The goal of a successful medicine isn’t simply to reduce mortality. Well-being is a key factor in patient outcomes, and with advances in the understanding of what contributes to wellbeing, clinical trials are adjusting their endpoints accordingly.
Well-being doesn’t only matter in relation to the final medical outputs of trials, either. The nature of the experience of a clinical trial is shifting towards a much more accessible and comfortable patient journey, which helps improve the rate and the accuracy of data they can report.
This means that clinical success relies on well-being in both trial and patient outcomes. Here are some of the other ways in which advances in psychology are affecting clinical trials:
- Risk – Socio-economic factors affect risk aversion in demographics targeted for clinical trials. This leads to a skewed sample of people from certain backgrounds who are more likely to balance the paid trial benefits favorably against the costs and sign up, and leads to deeper ethical considerations when designing trials.
- Patient-oriented approaches – A deeper understanding of patient care and wellbeing means that the design of clinical trials is changing to reflect the subjective nature of the experience from the patient’s side. Transparency and trust are two factors that psychology is showing the need to be prioritized in trials to maximize patient retention.
- Comfortable Patient Outcomes – A better understanding of the quality of life, as weighted against longevity, means that clinical waypoints and outcomes are changing to reflect well-being, rather than simply extending life. This also applies to the clinical trial itself, and qualitative experiences have been shown to boost trial benefits and impact decision-making.
As psychology advances its understanding of what makes people happy, the cold, objective nature of stereotypical clinical study grows more towards the comfortable subjective outcomes of a healthy mind for patients, as well as longer life, affecting the very design and efficacy of clinical trials as a whole.
These considerations are positively affecting patient retention, leading to smoother and faster completion of studies. As our understanding of what makes a therapy valuable, and what makes a trial comfortable improve alongside one another, future trials look set to continue this improvement.
Future of Clinical Research Technology
As medical science improves its understanding of physiology, and AI and machine learning enter a golden age, tech and medicine are able to facilitate one another to a previously unprecedented degree. With new hardware and software, the future of clinical trials looks good.
- Devices – Smaller, more powerful devices are being created all the time. There are now wearable heart implants that can connect to smart devices and function both as a recorder and a defibrillator for assessment and treatment. When connected to a network of other low-powered, implantable sensors, or even wearable tattoos, these devices create a Wireless Body Area Network that can send a comprehensive report to clinicians in real-time.
- Apps – A range of apps for both patients and clinicians is available to streamline the process of data collection, communication, and analysis. These can aid with selection, applicant tracking, and numerous well-being factors that we covered in the last section.
Apps also allow patients at home and in the clinic to connect directly to their devices via smartphones. This serves two purposes: it increases patient engagement with the study and facilitates real-time data offloading to the researchers. - Software – Between the devices and the apps, there is cutting-edge software. These make use of the tremendous modern capacity for data collection and analysis and mediate communications through various devices and the Internet of Things for rapid monitoring and diagnostics.
Machine learning is also applicable for patient selection, earlier identification of symptoms, and better outcome prediction, including for preclinical trials.

With unprecedented capacity for data processing, AI seems promising as a solution for combining the virtual chemical space with patient data to reduce the need for manual testing and cut the preclinical time down, while at the same time, providing might higher-potential chemicals for human clinical trials.
The data handling capacity is now waiting for quality data for training the advanced machine learning systems and as researchers shift to considering AI’s involvement in many stages of future trials, the motivation to produce data of the quality required should improve.
Participants in Future Clinical Trials
There are many physical and mental barriers to participants’ ability to report on the effects of clinical trials. Participants may not all be capable of communicating with the same degree of accuracy due to technological restrictions (e.g., in the case of using an app or a notepad) or might give differing reports because of the subjective nature of experience and differing vocabularies.
As such, reports of success or adverse reactions may be skewed by the subjective biases and limitations of using self-reporting methods. There are further limitations in current studies that prevent accurate measurements of some metrics of success such as effects at the molecular level.
Machine learning is improving upon these roadblocks in several ways, making the patient experience a lot less subjective, a lot faster, and more accurate, all that’s left to be done is to build up enough data for these systems to work with.
With advances in pattern recognition from data gathered from retinal scans and pathology slides, disease tracking could be faster and more accurate than ever. However, implementation is still delayed by the novelty of the technologies and the currently insufficient high-quality data required for such powerful tools to process.
There are proposals for systems that leverage the human neocortex, which is capable of learning from fewer data, which have been shown successfully in limited applications but have yet to be widely recognized.
Regardless, new analysis systems have huge potential in not only reducing the time a participant has to spend involved in the trial but boosting the accuracy of the feedback they can provide. This will improve a number of the challenges faced by clinicians and pharmaceutical manufacturers that relate specifically to follow-up data collection and applicant retention during trials.
The Future of Clinical Trials for Clinicians
The clinician’s role of finding, introducing, and supporting patients throughout the process of clinical development is one that requires tremendous skill and experience and an intelligent and robust strategy to execute.
Innovations like the Heart Bus from Astrazeneca bring compact and advanced diagnostic and analytic technology deep into the affected communities to be tested on-site. This has the potential for finding the right patients for clinical trials and saving significantly on the cost of retention by identifying better-fit patients and reducing the strain of their experience.
Advancements like this pave the way for further portable screening stations, where similar technologies can be applied to a wider range of diseases. These pre-screening processes can dramatically shorten recruitment time by rapidly identifying underdiagnosed diseases where they occur.

How Close are We?
There are so many ways in which the modern state of tech will aid clinical trials in the future. Much of the progress has already been made on the software, hardware, and social side of things – what remains is to break the inertia of the status quo and begin adopting new practices.
As it stands today, the future of clinical research is hindered by a lot of hesitation in employing modern approaches to clinical trials. Here are some of the major roadblocks relating to some of the examples we’ve covered in this article:
- For AI, there is a lack of viable data to train the system. Accessing data comes at a cost, and reliable data needs to be sorted from noise. It’s also not a widely understood process, meaning there is a lack of trained and skilled personnel who can operate the platforms. Finally, there are concerns around job security, relating to automation replacing workers, as well as skepticism around the reliability of a non-human entity to make correct conclusions on human-related topics.
For wearable devices, one of the issues is power consumption. While there are significant advances in this, cutting-edge devices are still particularly costly and in relatively low supply. - Security is another factor relating to devices, as communication channels need to be secure at the integration and data transmission points of the system. Technical difficulties from poor design quality are harder to work with when the device is implanted into a patient’s artery, and can in some cases create a negative patient experience if the device is unreliable.
- For clinical trial design, the major hurdles are with hesitance of investors to experiment with new approaches. With pharmaceutical companies competing to discover new drugs, revolutionizing a tried and tested process comes with a substantial financial risk; one that many aren’t willing to take.
Ultimately, it’s hard to say how close we are to reaching a more efficient system, but the components are almost all readily available to make clinical trials faster, more comfortable, and more successful overall, it’s simply a matter of learning to adapt to them.
Conclusion
Clinical trials are a long and expensive necessity for the production of safe and effective drugs. The slow and inefficient preclinical trial procedure, as well as the lengthy and rigorous human trial phases, contribute to a tiny fraction of tested compounds making it onto the market.
However, advancements in multiple sectors have created the potential for many of these processes to be automated, and for those that can’t, to be vastly improved in terms of speed and cost.
Further, better understandings of the nature of human experience have led to changes in desired outcomes and subsequently, overhauls in trial design.
The future of clinical research now depends on investors who are willing to take the necessary risks to adopt new approaches and we may soon welcome a new era of pharmaceutical discovery powered by AI, implantable devices, and powerful assessment tools, ultimately leading to a better quality of life for patients.