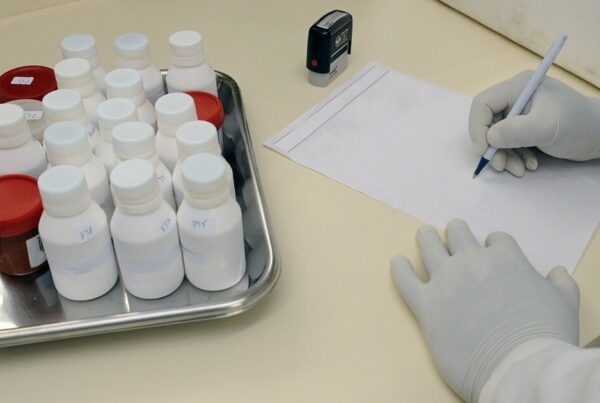
Centralized monitoring in clinical trials involves the collation of data from trial sites in a remote, central location.
- Feeling overwhelmed by managing data from multiple clinical trial sites?
- Worried about the efficiency and accuracy of your current monitoring process?
- Struggling to keep costs under control while ensuring data integrity?
With an increase in the technological reach of clinical trials leading to more complex, decentralized, and multi-site research, the most efficient way to handle the copious amount of data required and produced is by using a centralized monitoring system in conjunction with on-site practices.
This article is for:
- Clinical research professionals seeking to optimize their monitoring strategies.
- Drug development sponsors looking to improve data quality and reduce trial costs.
- Clinical trial managers seeking innovative solutions to ensure data integrity and patient safety.
The benefits of centralized monitoring are numerous, but this approach isn’t without its challenges. We’re going to take a look at the pros and cons of the system, and a brief overview of what it takes to get one up and running. To start with, let’s talk about what centralized monitoring means, and what it can do for modern clinical trials.
Centralized Monitoring in Clinical Trials: Understanding The Basics
Centralized monitoring, or central monitoring, involves data collection from multiple clinical trial sources in a remote, central location. It’s part of a more risk-based approach that regulators are pushing for sponsors to address the complexities that arise with the increasing number of remote and multi-site trials.
The purpose of central monitoring in clinical trials is to enhance monitoring data quality in an evolving landscape of trial design and is a growing trend over the past decade in response to increased data sets and a deeper need for collaboration, more complex monitoring plans, and modern technology to monitor modern trials.
This is a more statistical approach to handling information across multiple sites. The FDA defines centralized monitoring as “a remote evaluation carried out by sponsor personnel or
representatives (e.g., clinical monitors, data management personnel, or statisticians) at a location
other than the sites at which the clinical investigation is being conducted”, and strongly encourages its adoption where appropriate.
Part of this type of monitoring is the review of data submitted to assess it for quality, and a strong focus on addressing missing or inconsistent entries, outliers, or protocol deviations. With this form of monitoring in place, sponsors can analyze data sets to identify trends in numerous key metrics such as distribution, consistency, and completeness. This can help them pick out discrepancies in how protocols are being followed between sites or other contexts in which there may need to be an intervention.
It can be used to remotely monitor performance metrics, verify source data, and other value-adding processes to the clinical trial, without needing to rely on on-site monitoring processes. Next, we’re going to take a look at some of its applications in more detail.
Why the Need for Central Monitoring in Clinical Trials?
From the FDA’s non-binding recommendations, it’s suggested that clinical trial central monitoring can be used in two key contexts.
The first is to supplement or reduce the need for on-site monitoring.
This can be by executing routine reviews to monitor data quality, missing data, or protocol deviations, as previously stated, but extends to numerous other useful applications, such as:
- Identifying trends that can’t be detected with on-site monitoring – Centralized monitoring can spot red flags such as the unusual distribution of data between sites.
- Site performance metrics – Metrics such as a high-screen failure, or high withdrawal rates can help to identify low-performing sites and allow for earlier interventions to correct this.
- Complete admin and regulatory tasks – This could be comparing randomization and CRF data, or verifying IRB approval by remotely reviewing IRB correspondence. It can also be used to monitor consistency between sites when it comes to the receipt, administration, and reporting of the investigational product.
The second suggested application of centralized monitoring in clinical trials is the ability to target on-site monitoring by identifying higher-risk sites using the same above activities.
The majority of these techniques can be performed using CRF data, whether via an EDC or on paper. However, it’s suggested that the move to more digital forms of data capture and storage is not only a driver but also a facilitator of the need for and strength of centralized monitoring techniques.
Improved methods of data collection increase the amount and power of the data supplied, subsequently improving the ability of centralized monitoring, but also pushing for its use by adding the complexity that comes from increased data from multiple streams.
As decentralized trials are on the rise, therefore both opportunities and challenges for data collection and analysis present themselves. Before we get to these challenges, let’s dig a little deeper into the benefits.
5 Key Advantages Of Centralized Monitoring In Clinical Trials
The nature of a centralized monitoring system comes from its nature as a facilitator of convenient access to source data. With a single, centralized system that can be accessed remotely, there are numerous potential benefits and many are currently being realized by those who have adopted it.
1 – Efficiency
Removing the need for frequent site visits for source data verification saves tremendously on resources, and this benefit is compounded in trials that occupy numerous sites, especially internationally. This is also true for the implementation of adaptive trial monitoring within sites, and the efficiency boosts that come with the necessary shift to electronic data capture and management of source data.
2 – Range Of Participants
Multiple sites and data sources can be monitored from a single location, which greatly expands the reach of trials when it comes to finding participants. This benefit applies most strongly to trials that relate to treatments for rare conditions that may require multiple, distant sites, potentially across the world, to reach a powerful enough sample.
3 – Patient Safety & Data Quality
An ability to execute real-time risk monitoring increases patient safety and the ability to process these data in a way that improves its quality boosts outcomes both in terms of speed and reliability of the data. This leads to an increased validity of data collected via expanded data sets. With clinical trial central monitoring, both patient safety and data quality are enhanced.
4 – Resilience Of Trials Through Restrictions
One of the real tests to trials came during the pandemic restrictions, which greatly limited the ability for people to move and interact with sites. Multi-center trials that did not adopt centralized monitoring were hit particularly hard, and many were forced to make the change. This decision, in most cases, was the right one to make and has helped to boost the reputation of centralized monitoring as a solution to many issues faced in modern trials.
Collaboration & Faster Response Times
It is hoped that the ability for sponsors, CROs, and site staff to access and review the data in a centralized system in real-time will provide boosts to communication with site staff. Issues can be spotted earlier, and on-site monitoring can be prioritized to areas that are critical to the study, where needed. Where some sites are having difficulties, sponsors will be able to identify and take corrective action.
It’s clear that a picture of efficiency, better control, and faster response times is being painted by the proponents of centralized monitoring, but it isn’t without its challenges and limitations.
Challenges Faced In Clinical Trial Central Monitoring
The first disappointment that might arise in sponsors when it comes to implementing such a system is that the money saved in remotely monitoring sites over visiting them directly, is, at least, at first, offset by the cost of implementing the software.
In many cases, particularly where centralization is done internally, engineers will be required to program and process the information, and this will represent an increased cost that may be unappealing. This is typically the first hurdle to overcome, but there are others.
Centralized monitoring is most effective with electronic data and the need to switch to a more digital form of data collection creates its own issues. For example, the increased adoption of electronic patient-reported outcomes makes it important to ensure that patients are compliant when it comes to completing forms and questionnaires.
While some of these difficulties are actually simplified by the real-time data access that comes with centralized monitoring, there is still going to be a need for site visits and on-site monitoring practices.
Reasons for these include:
- Training of new staff, or of current staff in the new approach to monitoring and its corresponding data requirements.
- Product accountability, such as inventory calculations and monitoring storage of investigational products.
- Follow-up visits relating the queries around the data provided.
- Protocol assessments and similar management tasks
Clinical trial central monitoring is primarily a risk-based approach to monitoring in clinical trials. Therefore, while many of the benefits relate to efficiency and potential resource-savings, these need to be considered as secondary to the main purpose of identifying trends remotely and addressing problems quickly.
Finally, the major challenge faced when proposing a move to central monitoring comes from its apparent technical complexity. Sponsors may be immediately put off by the apparent complexity and technological hurdles involved in advancing to such a system, both in terms of financial cost and the learning curves anticipated in bringing the system online.
Therefore, the first step to overcoming these challenges is to demystify the process.
Centralized Monitoring Is Easier Than It Looks
As discussed, remote monitoring provides a platform for study teams to identify and respond to anomalous data trends, and thus improve the quality of regulatory submissions. As a result, it is strongly encouraged by regulatory bodies such as the FDA.
However, the development of this system has recently been accelerated by the growth of various technological facilitations that are pushing trials to become more data-driven than ever. This leads to the image of a CM system that requires in-depth and expensive expertise to implement and manage.
The adoption of a centralized monitoring system certainly does require some financial and intellectual output, but in reality, there are few processes involved that require skills outside the capabilities of anybody professional in the field of life sciences. As such, to overcome the very first hurdle of sponsor approval, it’s important to understand what it takes.
Planning a centralized monitoring strategy primarily requires a familiarity with risk management, followed by a fundamental understanding of statistical analysis. Again, these concepts should not be out of the reach of the majority of research professionals.
For the risk management components, it’s necessary to be able to identify risks, assess their potential impact, and come up with mitigation strategies based on how critical they are and the likelihood of them occurring. This is a relatively simple task that trial design will already involve.
Then, to perform the monitoring, a basic comprehension of statistical principles such as means, standard deviations, and how they can be used to detect outliers. A simple use of chi-squared distributions can be applied to detect scientific misconduct, which is a rare, but critical risk to manage.
Finally, it’s important to repeat that a CM strategy does not remove the necessity for on-site visits. Effective use of the system involves a mix of both remote and on-site monitoring practices and is a matter of devising a strategy that incorporates the strengths of each into a unified approach. Once sponsors are informed and on board, the process of working on a trial monitoring plan can be relatively simple.
Developing A Clinical Trial Central Monitoring Plan: Best Practices
So, what might the devising of a good monitoring plan look like? First, it should identify the various methods that will be used and why. The primary function of monitoring will be the mitigation of high-risk and high-likelihood events that relate to the conduct, collection, and reporting of essential data. It should also cover the critical processes for participant safety and trial integrity.
Remember that centralized monitoring needs to play to its strength. It’s not a catch-all for every kind of monitoring, and therefore needs to be considered as a tool for covering only the primary efficacy and safety variables that affect the study results.
As an overview of where to focus in risk-based monitoring, some suggested variables to track include:
- The number of important protocol violations
- The major protocol deviation rate
- The minor protocol deviation rate
Then, the key steps for implementing centralized monitoring are:
- Identifying and defining key risks and their thresholds for action.
- Designing a comprehensive monitoring response and the documentation associated with it.
- The continuous monitoring of risks and the use of the appropriate technology to aid this monitoring.
- Corrective action planning to mitigate or remove these risks
While this isn’t as simple as it might appear, it’s not profoundly complex either. Here are some best practices for designing and implementing a system that works.
Allocate The Right Central Monitor
Depending on how technological the current practices are, implementing a central management system in a clinical trial could involve a lot of unfamiliarity among those involved. Making sure the right level of experience is on hand is the first step to transitioning smoothly, and having a central monitor onboard with a background in monitoring and the appropriate knowledge of data management should be a top priority.
The central monitor should be involved in the primary risk assessment stages that will create the strategy and show regulators the reasons and motivations behind choosing a specific CM pathway. Central monitors, having a statistical background, need to be familiar with:
- The normal distribution
- Z-scores and p-values
- Cumulative probabilities
- Fraud detection
- Chi-squares distributions
They should also have good communication and organizational skills.
Find The Best Solutions For Your Technology Stack
While the human element is critical, the technological components are also significantly going to impact the design, use, and efficacy of the system.
Integrations are crucial to the success when it comes to dealing with multiple sources of data, as will the ability to handle the sheer volume coming in. Then, the UI needs to be friendly and easy to handle across a range of experience levels. Graphical representations should be clear and intuitive, and the tech needs to have been through a reliable validation process to ensure it’s secure and compliant with regulatory requirements.
Bring In All The Relevant Stakeholders
For all of this to work, there needs to be a group effort. Bringing in the relevant minds to the planning and implementation stages will help smooth the transition and identify the impacts, both positive and negative, on the people involved.
When running the system, open communication between on-site and remote monitoring teams is important to its efficacy, so bringing both into the planning stages together will help cement this relationship and set expectations for the communication required moving forward.
Conclusion
Central monitoring is essentially a risk-based approach to monitoring that improves anticipation and reaction time to numerous factors that can affect the safety or efficacy of clinical trials. It does this by offering real-time access to data from multiple sites and offering elegant statistical solutions to pick out unexpected trends.
However, this technological approach can be intimidating, so understanding what its implementation involves is the first step to overcoming the challenges it faces.
Despite all its benefits, it’s not a catch-all solution and will require critical thinking and expertise to bring into play, but with the right resources and policy design, and an inspired culture of open communication between stakeholders, the benefits can be effectively balanced against its limitations and risks.